The next few days will be related to hormonal changes and various symptoms we experience such as increased risk of osteoporosis, joint inflammation, allergies, headaches etc.
Peri to Post Menopause and the vaginal microbiome
Vaginal health affects many of us once we enter menopause and beyond.
The vaginal microenvironment is exposed to substantial modifications throughout a woman’s life.
It has its own unique community of microorganisms which is very different from the gastrointestinal tract microbiome and other microbial niches in the body.
Vaginal health is dependent upon levels of lactobacilli species. These are usually the more dominant and protective microbes keeping the vagina acidic (3.8-4.4 pH). If the community shifts to a more diverse community, the vagina becomes more alkaline which is not as protective and may lead to other symptoms. You can test the acidity of your vagina using strips which can be obtained on amazon.
These are the strains which should be dominant in a healthy vagina:
- Lactobacillus crispatus
- Lactobacillus iners
- Lactobacillus jensenii
- Lactobacillus gasseri
Several stressors, such as alternations in hormones and our habits, can dramatically change vaginal microbiome composition, resulting for example in the depletion of lactobacillus, reduction of microbial diversity and occurrence of dysbiosis, often leading to bacterial vaginosis, yeast infections, sexually transmitted diseases, urinary tract infections and poor fertility.
Dietary intake has been shown to play a role in influencing the composition of vaginal microenvironment in women of childbearing age, since a lower concentration of some essential nutrients, such as vitamins A, C and E, b-carotene deficiency and an altered iron status may contribute to the risk of bacterial vaginosis and Candida colonisation. At a similar extent, increased plasma glucose levels and dietary fat, as well as obesity, are associated with poorer vaginal health and dysbiosis state.
The composition of this microbiome is relatively stable during reproductive years, but levels of certain microbes may fluctuate with hormonal fluctuations.
Discharge ought to be normal and variable: clear to white, odourless, and of high viscosity.
Before you start the approach of the menopause, oestrogen will trigger the cervix into producing a mucus and this mucus is just very slightly acidic which is really important because that acidic mucus can help to restrain any bad bacteria or fungi that may actually inadvertently appear in the vagina.
Symptoms of reduced mucus:
Candida/Thrush:
If the mucus in the vagina decreases, that means that the level of acidity decreases as well, which means that other bacteria can get in, other fungi can get in and that can give you things like thrush, it can give you things like Candida and it can give you other bacterial infections of the vagina. A vaginal probiotic is one of the best things that you can use. Ordinary digestive probiotics will not help you. Remember the combination of bacteria in the vagina are very different so you need to get a specific vaginal probiotic.
Beneficial yeasts which can suppress candida growth are Saccharomyces cerevisiae. For thrush Boric acid pessaries may be the answer.
If antibiotics are needed don´t forget your probiotics and consider lactic acid douches and pessaries.
Vaginal Dysbiosis* – follow post later today on Sea Buckthorn oil
This is often characterised by symptoms such as: Itching, burning, general discomfort through to pain and burning, changes in discharge to watery, chucky cottage cheese like, coloured (grey, yellow, green, rust)
Smell: fishy, ammonia or rotten smells not encountered previously.
Cystitis and bladder infections:
If the level of friendly bacteria decreases in the vagina, that can have a direct effect on your bladder health and remember in the menopause your bladder tends to get weaker and more easily irritated anyway. If you lose the friendly bacteria in the vagina then that will leave you more vulnerable to infections such as cystitis and the problem here is we are often prescribed antibiotics and antibiotics kill off more of the friendly bacteria and that’s when we end up getting repeat bladder infections and that will weaken the bladder further. Ensure your water levels are up, take a vaginal probiotic and/or cranberry products to help to treat the infection and to help as a preventative.
Vaginal Dryness* see post later today
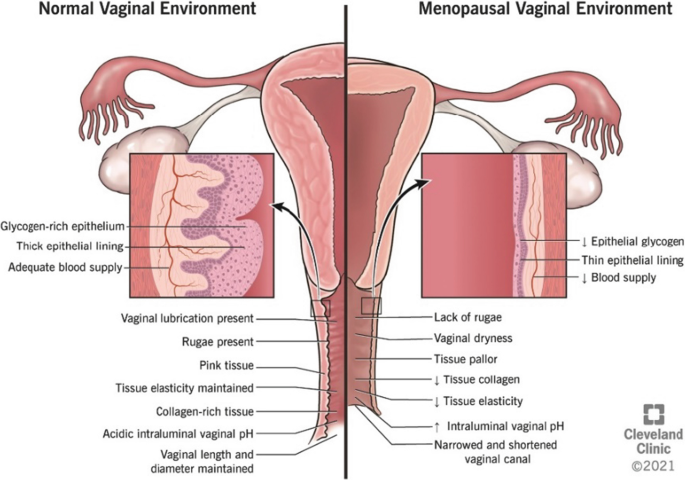
Vaginal secretions are greatly reduced in menopause once periods cease.
The lining of the vagina is very, very thin. So although it’s strong, if that thinness and flexibility gets affected because there is very little mucus, then the inside walls of the vagina they can become very brittle and they lose their elasticity and that can cause a lot of problems.
Bleeding or spotting and very often that is because the lining of the vagina has actually been torn or irritated or scraped during intercourse. So if you’re getting this spotting on a regular basis after intercourse, you know, that’s a good indication that there might be too much dryness.
Also in this situation, the minute the vagina starts to dry out, you can get irritated. This can lead to itchiness and inflammation and that can lead to more discomfort.
Support: a vaginal probiotic/seabuckthorn oil?
Thinning Skin:
For some women the skin can get so thin on the vagina and also the vulva area that you end up with nerve pain and this can be really difficult to sort.
What can you do? Massage oil/cream twice a day to keep the skin supple.
Vaginal Atrophy:
The vagina and the vulva are usually rich in oestrogen receptors, so when oestrogen levels are reduced and not as much is attaching to the oestrogen receptors, physical changes such as atrophy (loss of size) of the vagina and vulva can occur. In fact oestrogen and collagen reduction means that skin thickness is likely to decrease by up to 30% in the first five years post menopause.
Ask your doctor/gynecologist for local oestrogen/oestrogen cream if all else fails. Don’t suffer in silence. This is a very common issue.
Change of smell?
You will for some women find that the mucus, there’s a change of smell too.
Very often this is just due to a change in the levels of the bacteria in the vagina and this one can usually be put right quite quickly by using a probiotic.
You might find that your vaginal mucus or discharge gets more sticky, it might get more runny, it might change colour. This tends to be due to the hormones and this is very common when you get to the peri-menopause where your oestrogen and progesterone levels are still in a bit of a cycle.
If your oestrogen is starting to go really high, (oestrogen triggers the cervix to produce mucus), then the cervix can be over-stimulated and you can end up producing a lot of mucus (almost like having a non-blood period), and very often that’s just due to the fact that your oestrogen is running a little bit out of control.
Agnus castus and probiotics may be supportive.
If in doubt get it checked out – Don´t suffer!